Nearly five years ago, Rae wrote the birth story for her third child, Gideon. He was very poorly when he was born and spent time in NICU and SCBU. At that time, she didn’t really have any answers and didn’t know what the future might hold. Since then Gideon has been diagnosed with Prader-Willi Syndrome and life has taken the family on a very unexpected journey. Rae has written a mini series of blog posts for Take 5 and chat, and she raises some important issues and offers some helpful suggestions. Thanks Rae.
If you’ve had a baby in NICU (Neonatal Intensive Care) or SCBU (Special Care Baby Unit) you are part of a special club – one that actually, you don’t want to belong to. Getting to grips with the special language is the least of your worries. It’s a whole new way of life and support from friends and family is vital. I will never forget the people who carried me when Gideon was first born.

- Keep in touch – but don’t expect replies. It is lovely knowing that people are thinking of you and to get news from the outside world. Even the most mundane of updates are great. So keep the text messages coming. It can be hard having to give the same updates to multiple people too, especially if there is no news, or even worse, bad news. It might help to offer to set up a news chain, so you pass on agreed information to other people.
- Visit – it might not be possible, it might not be allowed. But if you can manage it, please try. When Gideon was first born and very ill, I wanted as many people to visit him as possible. I knew that if he did die I wanted as many family and friends as possible to have met him and for the funeral not to be the first and only time they saw him.
- Coffee breaks – even if you can’t visit the ward, meeting in the hospital for a cup of coffee is a lifeline. Seeing other people, possibly even talking about other things is vital.
- Hand cream – bring in some basic, or lovely hand cream, as hands are washed all the time and can become very dry.
- Food parcels – there’s no getting away from it: hospital food is shit. Worse than school lunches. So if you can bring in something homemade and delicious you will be elevated to hero status. And if you can’t manage that then a Marks and Spencer salad or snack pot will be just as good. Or even some vouchers for the coffee shop.
- The cost of having a baby in hospital soon adds up too – having had an emergency caesarean I wasn’t meant to be driving but I needed to get to hospital and back. My husband was at home looking after the big two. I certainly wasn’t up for public transport, so I relied on lifts and taxis. After that I used public transport and when I did start driving again (two weeks after he was born) I had to pay extortionate city centre parking tariffs. So, any lifts or change for the metro or for parking machines would be very well received.
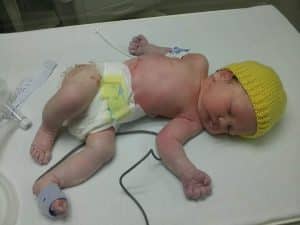
Look out for Rae’s next blog post coming soon! Take 5 and chat would like to thank Rae for writing for us, and we also thank all the amazing people who support parents caring for children in hospital.
Prader-Willi syndrome (PWS) was first described in 1956 by Swiss doctors, Prof. A Prader, Dr A Labhart and Dr H Willi, who recognised the condition as having unique and clearly definable features. These features are, as medically described:
- Hypotonia: weak muscle tone, and floppiness at birth.
- Hypogonadism: immature development of sexual organs and other sexual characteristics.
- Obesity: caused by excessive appetite and overeating (hyperphagia), and a decreased calorific requirement owing to low energy expenditure levels. (Obesity is not normally a feature of those whose food intake is strictly controlled.)
- Central nervous system and endocrine gland dysfunction: causing varying degrees of learning disability, short stature, hyperphagia, somnolence (excessive sleepiness), and poor emotional and social development.



